Hiatal Hernias
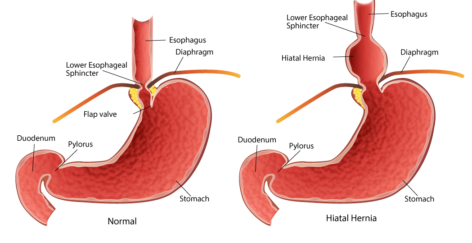
A hiatal hernia, also known as a diaphragm hernia or paraesophageal hernia, is a medical condition where the upper portion of the stomach pushes up through an opening in the diaphragm and into the chest. The diaphragm is the thin muscle wall that separates the chest cavity from the abdomen. The natural area where the esophagus goes through the diaphragm is called the hiatus - which is where the stomach commonly pushes through the diaphragm.
A small hiatal hernia usually doesn't cause problems. Many people never know they have one until their doctor discovers it while checking for another condition.
Moderate and large hiatal hernias, on the other hand, can change the structure of the stomach and affect your ability to keep food and stomach acids where they belong. With a hiatal hernia, food and acid can back up into your esophagus, causing heartburn. Although medications and other self-care measures can usually provide symptom relief, they will not stop the mechanical problem caused by the hernia. Large hiatal hernia can also cause significant problems breathing as the stomach is taking up ‘room’ in the chest cavity, pushing the lung aside. Hiatal hernias tend to get bigger with time and many ultimately at some point may need an operation.
Types of Hiatal Hernias
There are two different types of hiatal hernia. The type you have will determine if closely watching it will be enough or if surgery is most likely needed.
Sliding Hiatal Hernia
Sliding hiatal hernias are the most common type accounting for 95% of all hiatal hernias. With a sliding hiatal hernia, your stomach and the lower part of your esophagus slide in and out of your chest through the diaphragm, hence the name. This type of hiatal hernia is especially common in smokers, overweight people, and women older than 50.
Fixed Hiatal Hernia
In paraesophageal or "fixed" hernias, the stomach pushes through the hiatus into the chest area beside the esophagus and stays there. Paraesophageal hernias are more likely to cause more severe symptoms than sliding hernias and can cause blood flow to be cut off to the stomach if not fixed by a surgeon.
Symptoms of a Hiatal Hernia
Many people with a hiatal hernia never have symptoms, but when they do, they are similar to the symptoms of gastroesophageal reflux disease (GERD). GERD occurs when digestive juices move from the stomach back into the esophagus. Symptoms of GERD include:
- Discomfort or pain in the chest or stomach
- Heartburn
- Trouble swallowing
- Coughing
- Regurgitation of food or liquids into the mouth
- Backflow of stomach acid into the esophagus (acid reflux)
- Shortness of breath
While these symptoms could be related to conditions other than a hiatal hernia, it is important to see your doctor if you have any persistent signs or symptoms that worry you.
Diagnosing a Hiatal Hernia
To diagnose a hiatal hernia; your doctor may do tests including:
- Barium swallow. Involves drinking a chalky liquid that coats and fills the inside lining of your digestive tract. The coating shows up on an X-ray, allowing your doctor to see a silhouette of your esophagus, stomach, and upper intestine.
- Endoscopy. A thin, flexible tube equipped with a light and camera (endoscope) is placed down your throat to examine the inside of your esophagus and stomach and check for inflammation.
- Esophageal manometry. A different kind of tube goes down your throat to check the rhythmic muscle contractions in your esophagus when you swallow.
Treatment Options for Hiatal Hernias
Many people with a hiatal hernia don't experience any signs or symptoms and won't need treatment. Those who do experience symptoms, however, may need medications or surgery to give relief.
Medications to Treat Conditions Caused by a Hiatal Hernia
It is common for someone with a hiatal hernia to have GERD. If you experience symptoms such as heartburn and acid reflux, your doctor may recommend:
- Antacids that neutralize stomach acid
- Medications to reduce acid production
- Medications that block acid production and heal the esophagus
The medications will decrease the amount of acid made in the stomach and will many times help alleviate the symptoms, but will not take care of the mechanical issue of constant reflux. The hiatal hernia must be repaired to completely repair the GERD issues.
Long term GERD medication use has also been shown to have a number of side effects including osteoporosis, increased bone fractures, and increased risk of developing Alzheimer's disease.
Surgery for Hiatal Hernias
Sometimes a hiatal hernia requires surgery. If you’re experiencing regular reflux and other discomforts, or if the hernia is causing complications such as severe inflammation or narrowing of the esophagus, Dr. Howard may recommend a surgical approach.
Surgery to repair a hiatal hernia can be done in a few different ways, depending on what the surgeon sees. The majority of time the major portions of the surgery include:
- Pulling your stomach down into your abdomen
- Removing the hernia sac
- Making the opening in your diaphragm smaller with suture
- Sometimes using a biologic (resorbable) mesh for extra reinforcement
- Reconstructing the esophageal sphincter with a natural wrap of the upper part of the stomach like the Nissen fundoplication or using a mechanical device like the Linx
The vast majority of the time Dr. Howard can do this laparoscopically, only on rare occasions does an open surgery have to be performed. Dr. Howard will discuss which technique might be best for you.
If you have been diagnosed with a hiatal hernia and would like more information regarding your treatment options, contact us today to schedule an appointment with Dr. Howard at our office in The Woodlands, Texas.